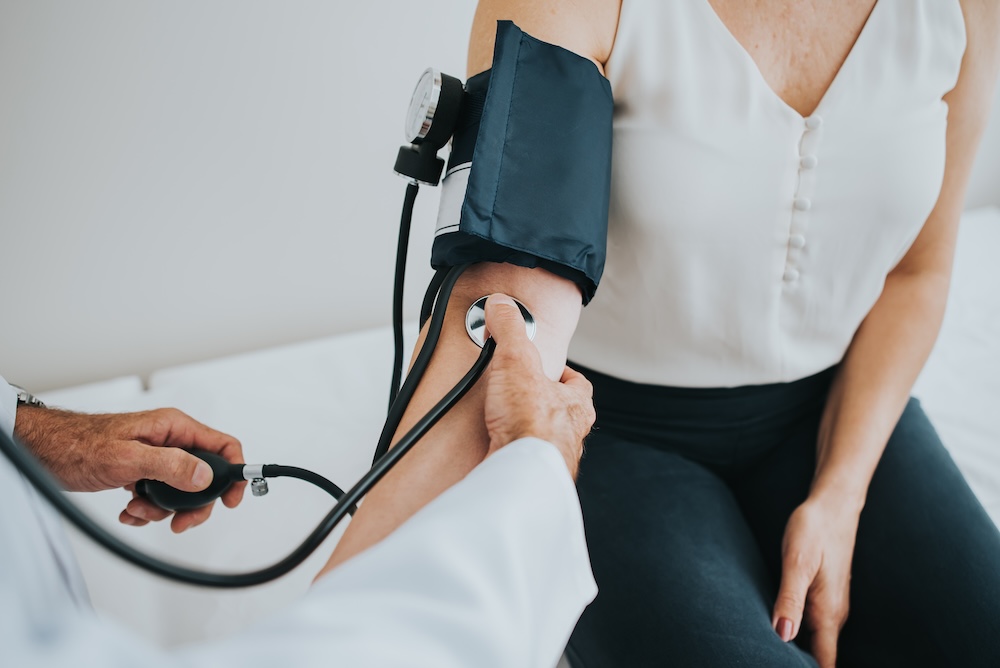
The menopause experience of people of color is under-researched and poorly understood. They can have more intense menopause symptoms, yet don’t get the right treatment options or appropriate care. It’s important to understand why this happens and to find ways to bridge the gap in knowledge and personalized care. Read on to find out more.
Find what you need quickly
Stories from the consultation room
Delilah wondered why she seemed so short with her husband and 10-year-old daughter over the last few months. As a 43-year-old woman in a fast-paced, stressful job, she chalked up the increased irritability to increased work demands.
The only other time in her life that she felt her mood shift was following the birth of her daughter. At the time she’d suspected she had postpartum depression but was told by her midwife that she was likely just exhausted from the demands of being a new mom. But now the fluctuating moods were back.
“It wasn’t just the mood stuff that bothered me,” Delilah said during our first consultation. “I couldn’t sleep. I would wake up and feel wired. And then I started having sweats.”
She’d heard that night sweats could be related to perimenopause but wasn’t sure. She had gone first to her medical doctor to ask questions about her bothersome symptoms. “She simply told me that I needed to lose weight, and that my stress was likely related to my job and I needed a vacation. She gave me a prescription for a sleep medicine. I never fully got my questions answered.”
Delilah’s story seems pretty straightforward – she is a middle-aged woman with early-onset symptoms of menopause. Yet, it mirrors the experience of many women of color when accessing menopausal care:
- Symptoms are minimized
- Lower likelihood of being offered treatment options
- Ongoing disconnect between patient needs and healthcare provider response
What is menopause like for women of color?
Data from the Study of Women Across the Nation highlighted stark differences in the menopausal experiences of women of color versus white women in the United States. Black, indigenous and other people of color (BIPOC) were more likely to experience perimenopause, or the time leading up to the final menstrual period, sooner and with longer-lasting symptoms.
These women were also more likely to have more severe symptoms and experience an earlier menopause.
Yet these women are also less likely to be offered treatment options. This includes hormonal treatment (HT), which is an effective treatment for some menopause symptoms. It can also help reduce cardiovascular disease and protect bones.
Why are women of color not getting the right treatment?
Understanding the reason behind these disparities in care is crucial to moving forward and improving menopause care for women of color.
Lack of training
A 2019 study highlighted the inconsistent training of healthcare professionals in menopausal health. Only 20% of the survey respondents reported that they had any training and just 7% said they felt comfortable caring for menopausal patients.
All obstetrician-gynecologist programs require some education on treating patients during menopause and beyond. But we are lacking the breadth of training needed to address the physiological and psychosocial aspects of menopause.
Lack of specialists
The North American Menopause Society offers training and certification for multi-specialty clinicians dedicated to treating patients in menopause. There just aren’t enough menopause-trained clinicians to meet the demand of patients requiring this specialized, patient-centered care.
The role of bias
Implicit bias happens unintentionally and automatically, affecting judgments, decisions and behaviors. In turn, this impacts the care patients receive – Black women are the least likely to leave the office with a prescription for hormone treatment.
There are preconceived biases around the affordability and desire for hormone use. Patients can be dismissed for simply being considered too young for menopause even with ample data showing that Black women experience menopausal transition earlier and have higher rates of early menopause.
This implicit bias from healthcare providers affects:
- Patient trust
- How open a patient will be during a consultation
- Patient compliance
It’s so hard for patients to know when and how to advocate for themselves in the perceived provider-patient power dynamic.
What can you do to improve your menopause experience?
Menopause receives less attention and structured learning compared to puberty and pregnancy. Preparation, partnership and community can help you feel empowered during menopause, even despite the physical and emotional unknowns. A 2018 study revealed that having formal menopause education can positively impact your experience and reduce symptom severity.
Improve your knowledge
Thankfully, we are seeing a menopause renaissance. Topics like hot flashes and vaginal dryness are no longer taboo and are getting the attention they deserve. Arming yourself with credible information is a great first step to increasing your knowledge. Read patient-friendly resources, such as the North American Menopause Society, to give you an overview of the baseline symptoms you can expect and how they impact your overall wellbeing.
Find the right clinician
Partnering with a clinician that centers your unique, individual needs can also support an empowering menopause experience. Menopause Society Certified Practitioners (MSCPs) receive comprehensive training on the menopausal transition and beyond and are required to stay up-to-date on the latest advances and technology in menopausal health through the maintenance of certification programs. You can find an MSCP on the North American Menopause Society website.
You can also explore menopause-specific benefits with your health insurer. Stella is a virtual clinic for menopause support offering everything you need to manage your symptoms, which includes access to clinicians, lifestyle support, and hormonal treatment (HT) if it’s right for you.
Trust yourself
As you navigate your patient-provider relationships, you may at times feel unheard or desire a second opinion. Trust your instinct. If you feel something is missing or you’re not being heard, consider seeking a second opinion with another provider.
Be prepared for your consultation
Keep a note of your list of questions before you visit your healthcare provider. This can act as a great prompt when in an intimidating setting, such as a consultancy room. The old paradigm of “doctor knows everything and patient knows nothing” is just that – old! Prioritize shared decision-making with your clinician and keep your personal goals front and center.
Get support from others
Make the most of your community. Any person with a uterus and ovaries will go through menopause and that’s more than half of the population! You shouldn’t have to go through this alone.
Being in a community provides you with validation for what you are experiencing, especially when so much of what we see about menopause in the media seems like a source of comic relief. Talk to your trusted friends and family members about what you are experiencing. Chances are that they may be going through the same journey as you if they are in midlife.
Final word
No matter who you are or what your experience with menopause is, you deserve to feel empowered throughout this journey. You have the power to rewrite the narrative even when the data shows concerning trends in how women of color experience menopause and how they are treated. Through the twists and turns or unexpected challenges that may arise from your menopausal transition, rest-assured that you’ve got this!
Find out more about menopause on our blog or in our symptoms library.